Benign breast disease
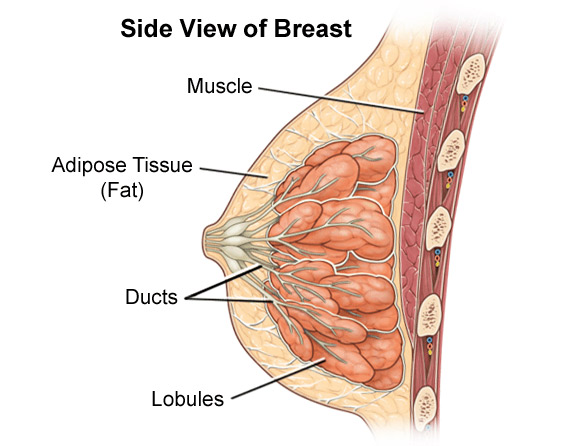 Benign breast disease is a term for a group of breast diseases that are not cancer. Because the first signs of breast cancers are frequently vague and ordinary, such as the appearance of a lump in the breast or an unusual discharge from the nipple, the causes of these signs are often found not be cancerous, but to be the result of a grab-bag of medical conditions that physicians call “benign breast disease”.
Benign breast disease is a term for a group of breast diseases that are not cancer. Because the first signs of breast cancers are frequently vague and ordinary, such as the appearance of a lump in the breast or an unusual discharge from the nipple, the causes of these signs are often found not be cancerous, but to be the result of a grab-bag of medical conditions that physicians call “benign breast disease”.
Even though most of the time the causes of these signs are found to be harmless, by conscientiously watching for these signs, and bringing them to the attention of a physician, women possess one of the most powerful tools that we have for finding breast cancers at smaller, and thus more curable, sizes. However, when a physician’s analysis of these signs leads to a diagnosis of benign breast disease, the most important message for the woman should be reassurance, because this indicates the absence of an important life-threatening illness.
Symptoms and signs
The signs of benign breast disease may manifest through various symptoms/complaints in many women. Common complaints include:
- a solitary (single) lump or thickening,
- multiple (many) palpable abnormalities,
- focal (easily located) or diffuse (widespread) breast pain,
- nipple discharge,
- skin discoloration,
- or skin dimpling.
The breasts also respond to many normal changes including cyclic changes from the menstrual cycle, changes associated with pregnancy, hormone replacement therapy, weight gain and/or loss, and aging. These symptoms are anxiety provoking because breast cancers may appear with similar symptoms. However, after appropriate medical follow-up, these symptoms are often found to be secondary to the various benign breast conditions that are referred to as “benign breast disease”.
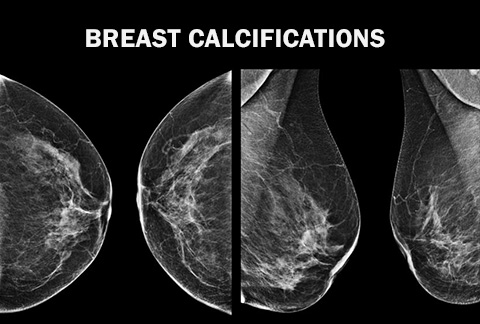
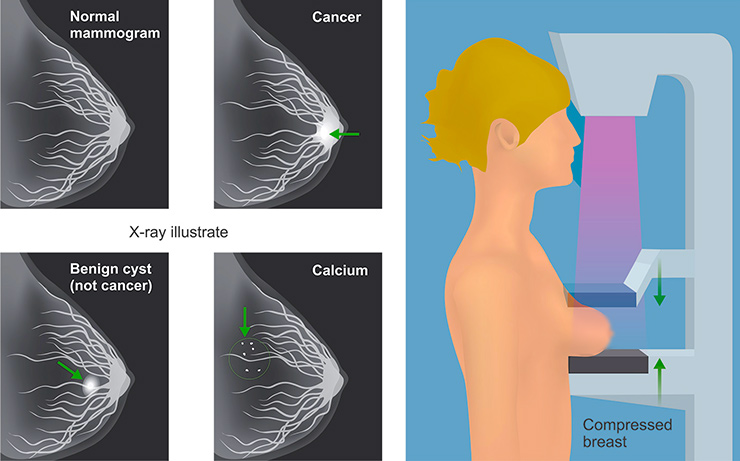
The signs of benign breast disease may also appear on a mammogram taken of a woman who has no other symptom. When the term “benign breast disease” is used in this context, it often describes mammographic findings, either a mass that can be seen on the X-ray film or as the small white specks that radiologists call “breast calcifications“, which often appear as a secondary result of a benign process.
The analysis of the signs of breast disease takes great skill on the part of the primary care physician, and, if required, on the part of the mammographer or radiologist (the doctor who orders and examines the mammogram), the surgeon (the doctor who will take a piece of breast tissue for analysis, if required), and the pathologist (the doctor who will examine the tissue under the microscope).
Types of benign breast conditions
- Fibroadenomas
- Cysts
- Galactocele
- Intraductal papillomas
- Lipoma
- Hyperplasia (typical and atypical)
- Sclerosing adenosis
- Radial scars
- Phyllodes tumor
- LCIS
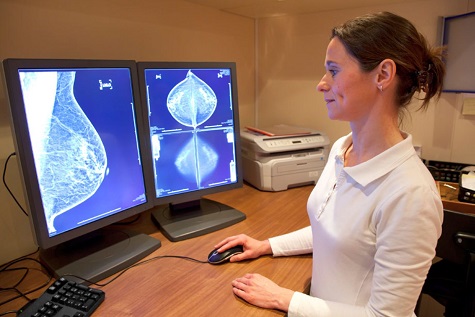
Mammography
If the signs of benign breast disease appear first on the mammogram. A mammographer may diagnose a patient with benign breast disease if certain types of masses or calcifications (small white specks) are identified on the X-ray film. Occasionally, a mass commonly described as a “spot” or “density”, will appear on a mammogram and have certain features, which enables benign diagnoses to be made with certainty. Similarly, calcifications, which are depositions of calcium into various tissues within the breast, may display a pattern, which the mammographer will identify
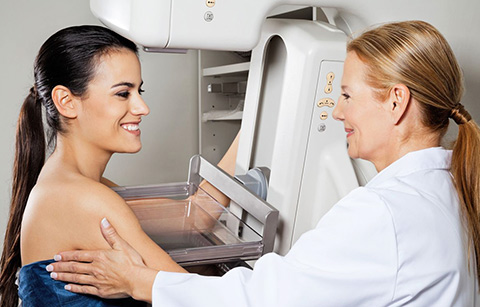
If the signs of benign breast disease appears first as a palpable mass. A common breast lump or thickening (which the physician will call a “palpable abnormality”) is the most frequent complaint in a woman presenting for a diagnostic mammogram. A new breast lump triggers a large amount of anxiety. Although most breast lumps are found to be normal after further evaluation, a woman should see a physician if she detects a palpable abnormality.
Often, a woman may find the lump or thickening by performing a self-breast exam. She will go to her physician who will then perform a complete clinical breast examination. The other common scenario is an apparently healthy (asymptomatic) woman who visits her physician for a different reason, and is found to have a palpable abnormality. In both instances, an experienced physician or nurse practitioner examines the patient’s breasts to detect any associated findings such as nipple discharge, skin discoloration or skin dimpling.
A woman is then often referred to the radiology department or practice for further evaluation, which often consists of a mammogram, and may also sometimes include an ultrasound targeting the palpable abnormality. Both the mammogram and ultrasound are complimentary examinations. The primary role of ultrasound is to determine if a lump is solid or cystic.
Solid vs Cystic
A cyst is a fluid-filled space within the breast. Cysts probably form as a result of an imbalance between secretion and resorption of fluid within the breast. A breast cancer is rarely found within a cyst. If a cyst fulfills certain criteria on ultrasound, it is classified as a simple cyst. No further follow up or work up is necessary.
If a cyst does not fulfill these criteria, then it is labeled as a complex cyst. In this setting, a cyst aspiration is recommended. This simple procedure entails placing a needle into the cyst and withdrawing the fluid. This procedure is performed to ensure that the cyst is not masquerading as a solid mass. Also, the fluid may be sent for cytology where it is examined in a laboratory to exclude the possibility of breast cancer.
A solid mass may be found under ultrasound examination to account for the palpable abnormality. The mammographer will evaluate the characteristics of the solid mass. The most common solid breast mass is a fibroadenoma; this benign and generally harmless tumor is composed of fibrous (structural) and glandular (milk producing) tissue. On ultrasound and occasionally on a mammogram, such a mass is oval in shape, has well defined margins, and is uniform in echogenicity (color). This mass may be monitored closely by physical examination, with a follow up mammogram and/or ultrasound in six months.
The management of this mass usually depends upon its size, and if prior radiological studies are available for comparison. If the patient or the referring physician desires diagnostic certainty a biopsy may be performed. A biopsy entails taking small samples of the mass, so that the pathologists (who are the tissue specialist) may make a diagnosis. Similarly, a woman may elect to have the entire lump removed. In this case, a surgeon would perform an open biopsy, usually same day surgery with anesthesia.
If a suspicious mass is identified which corresponds to the palpable abnormality, further evaluation consists of a biopsy or an excisional biopsy as outlined above.
Often the mammogram and ultrasound may not detect an abnormality. In this case, it is important for a woman to follow her referring physician’s recommendation. A woman may be sent to another physician who is trained in clinical breast examination for a second opinion. A fine needle aspiration may be performed. In this procedure, a small needle is placed into the palpable abnormality, and some cells (tiny amounts of tissue) are obtained, and sent to the pathologist for evaluation. Most often, a woman is monitored closely by her referring physician. If the palpable abnormality is stable, usually over a two-year period, then it is considered to be benign. If any changes in the palpable abnormality are identified, e.g. it becomes larger or painful, the woman is instructed to return to see her physician.
Pathologist’s examination
To the pathologist, who examines specimens of breast tissue, the benign breast diseases can be placed into two general categories: neoplastic (which indicates the growth of cells), and non-neoplastic. The non-neoplastic disorders are much more common than neoplastic disorders and encompass a broad and diverse group of conditions.
The most common non-neoplastic conditions are fibrocystic changes, radial scars, acute mastitis, and galactoceles.
Fibrocystic change
Fibrocystic change is the most common term that women hear in relation to benign breast disease. Like the larger category of benign breast disease to which it belongs, fibrocystic change contains a variety of sub-conditions. Frequently, fibrocystic change may have the external appearances of swollen, lumpy, and tender breasts. These symptoms frequently worsen just before a woman’s menstrual cycle begins and subsides near the end of the cycle.
If a piece of tissue (a “biopsy”) is taken, fibrocystic change may have a number of the internal appearances when analyzed in the microscope by a pathologist. Confusion arises because a woman may undergo a biopsy for a lump (a “palpable abnormality”) and be diagnosed with fibrocystic change or fibrosis. When this diagnosis is made, the woman can be reassured that her condition is not cancer.
Fibrocystic changes of the breast which generally affects women between 20 and 50 years of age who have not yet entered menopause, is the single most common disorder of the breast and accounts for over one half of all surgical operations of the female breast. Fibrocystic changes take on a great variety of appearances upon microscopic examination, which run the gamut from those that consist principally as cysts, to those that consist of increased amounts of ordinary connective tissue (fibrous stroma or fibrosis), to conditions that consist of increased amounts of the normal glandular (milk producing) elements of the breast (adenosis, and epithelial hyperplasia), and to conditions that have both increased stromal (structural) and glandular elements (sclerosing adenosis).
While not harmful in themselves, for reasons that are not understood, women with fibrocystic changes may be at slightly higher risk for breast cancer in the future, and should, therefore, be especially attentive to their annual screening mammography examinations.
Fibroadenomas
Fibroadenomas are second only to fibrocystic changes as the most common benign condition of the breast. This condition occurs most frequently in women less than 40 years of age and usually presents as a well-defined palpable mass. Microscopically, the mass consists of both epithelial (surface) and stromal (structural) cells with the latter cell type being most prominent. These masses are easily removed surgically and do not recur.
Radial scars
Radial scars (or radial sclerosing lesions) have been detected in 2-28% of benign breast specimens and present as both palpable and non-palpable masses. Radial scars are microscopic structures deep within the breast, and are unrelated to the normal superficial changes in breast appearance that may develop as women age. Radial scars are a benign condition that may sometimes be difficult to clinically and mammographically distinguish from cancer.
The cause of radial scars is unknown and may fall within the spectrum of fibrocystic changes. Like fibrocystic changes, women with radial scars, while not harmful in themselves, may also be at slightly higher risk for breast cancer in the future, and should also be especially attentive to their annual screening mammography examinations.
Acute mastitis
Acute mastitis (or breast infection) and galactoceles occur almost exclusively in lactating women. Acute mastitis and is thought to develop as a result of a cracked nipple which serves as the portal of entry for bacteria.
Galactocele
Galactoceles also occur during lactation and represent a cystic dilatation (stretching) of a single duct or multiple ducts. Secondary bacterial infection of galactoceles can convert this condition into foci of acute mastitis with subsequent abscess formation.
Intraductal papillomas
Intraductal papillomas occur most frequently in women in their 50’s and 60’s, and are the most frequent cause of both bloody and non-bloody nipple discharge. The term papilloma is used by pathologists to describe benign masses that form tree-like structure visible in the microscope; the papillomas seen in the breast are superficially similar to the more familiar papillomas, or warts, of the skin, and are equally harmless. Papillomas are generally solitary and located in the subareolar (nipple) region or major ducts.
Other less common benign neoplasms include pseudoangiomatous stromal hyperplasia, hamartomas, and hemangiomas. None of these conditions are life-threatening.