Pain relief for labor and delivery
Labor is the process by which the uterus contracts, the cervix dilates and finally the baby descends the birth canal. Delivery is the process by which the baby leaves the mother. Labor starts with regular contractions of the uterus (onset of labor). Pain is experienced with each contraction.
There are three considerations when one chooses the methods for pain relief during labor and delivery:
1) In labor, the opening of the cervix dilates from 0 to 10 centimeters (cm) and this takes an average of 8 to 12 hours for the first delivery, 6 to 8 hours for subsequent deliveries. Pain associated with this stage is mainly from the contraction of the uterus. For the time when the cervix opens from 0 to 3 or 4 cm, you are still fresh and probably can withstand the pain of each contraction. Normally, you do not need to take drugs for pain relief, non-pharmacological management described below, will suffice. As pain signal from the uterus goes through nerves connected internally to the spinal cord at the level of your lower back, if drug for pain relief is needed, it is achievable only by injections or by nerve block at the level of your lower back.
2) The baby’s head must descend the birth canal and it may take an additional 2 more hours after the cervix is dilated to 10 cm before birth of the baby. The main source of pain is from both the contraction of the uterus and distention of the vagina. Pain of contraction is most intense at this time. Medication by intramuscular injections or by nerve block is still the only effective management for you, if you find other methods are inadequate for pain relief.
3) An additional source of pain is from the stretch and sometimes tear of the vaginal opening during delivery. As soon at the child is delivered, the contraction of the uterus will stop. At delivery, pain at the vaginal opening can be effectively blocked by local injection of anesthetic drugs. This is the only time when a local anesthetic block can be successful.
The baby’s head is normally the first part delivered out of the birth canal. In case the pelvis or the legs of the baby presents itself ahead of other parts of the body, it is called breech presentation. In breech presentation labor pain may be more intense and instrument may be needed for delivery; both of which calls for more effective methods of pain relief.
Methods of pain relief
Pain relief is achieved by either distracting the patient, or by blocking the nerve fibers of the patient so that pain signals do not reach the patient’s brain.
Pain medications
You can be prescribed with various types of medication for labor pain. The most frequent medicine used is Demerol (also known as meperidine or pethidine), morphine, fentanyl, butorphanol and nalbuphine. The most effective route of administration is by intramuscluar injection, about once every 4 hours. It may cause constipation, nausea and vomiting, more so in a pregnant patient whose ability to empty the stomach is limited (that is the reason why you get heart burns during pregnancy).
Addiction to the opioids given (Demerol is a narcotic) is extremely unlikely as only a few doses are given for relief of pain and not for recreation. The baby born to a mother who has received opioids within 1 hour or so are depressed: has slow respiration, takes a longer time to give the first cry, or moves sluggishly. If the newborn is helped properly, within 5 to 10 minutes after birth, it behaves as normally as newborns without exposure to opioids.
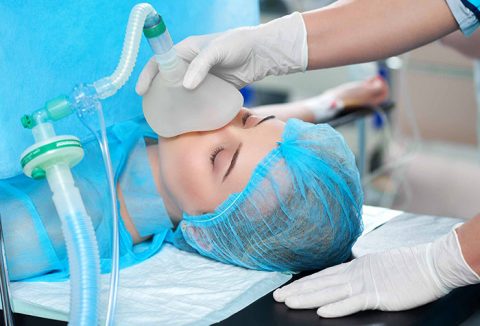
Epidural anesthesia
Continuous epidural anesthesia (commonly known as epidural) is a very effective method of pain relief. It is given for labor pain only after labor is established (i.e. you do not have a false labor). It involves placing a small needle into your back at the level of your waist and depositing anesthetic drugs outside the sac which contains the spinal cord.
An intravenous (IV) must be started to give you about 500 cc of solution. This is done to minimize the drop in blood pressure which is a side-effect of epidural . You will be asked to either sit-up, or lie on your side. You must curl up so that the gap between the bones in your vertebrae is opened as wide as possible. This facilitates the epidural needle to go through. A dose of anesthetic drug is deposited with the epidural needle. For a Continuous Epidural, a small plastic catheter is placed through the needle and left in place after the needle is removed.
It takes about 10 minutes to have the intravenous done and the infusion of 500 cc solution. The process of inserting the epidural takes about 10 minutes and the drug takes about 10 more minutes to become effective. Therefore, from the moment the decision to perform an epidural for a patient is made to the time when the patient first gets relief, it takes at least half an hour.
Side-effects and complications of epidural
common side-effects:
- drop in blood pressure: can be minimized with fluids and treated with medication
- shivering: happens to 1 in 3 patients after an epidural, can be treated with medication
- loss of sensation: some patients dislike the feeling of losing sensation and feeling no urge to push because she does not know when contractions come. To some of them, Freedom from labor pain is not as important as being able to feel the urge to push with each contraction.
common public concerns:
- “Epidural is associated with higher incidence of forceps delivery or Cesarean Sections”
The statement is correct but it does not demonstrate that epidural causes more forceps delivery or Cesarean Sections. A delivery which requires instruments or operation is likely the result of a difficult labor (e.g. prolonged labors, breech presentation, inductions ). It is not suprising that an epidural is requested in such case. - “Epidural causes back pain after delivery”
We have described earlier how the epidural is done. The epidural needle goes in through skin, fat, muscles, ligaments, and in the space between two pieces of bone. It does not go through bone, discs, or joints. It is therefore difficult to imagine how an epidural could have caused back pain. Furthermore, about 1 in 3 patients experiences back pain regardless whether epidural was used or not. - “Is the baby affected by the epidural?”
Epidural is by far the most effective method of pain relief. In fact, with a strong dose of medication, Casarean Sections could be performed with epidural anesthesia. However, epidural is so effective only because it is given in the vicinity of the spinal cord. The dose of medication the mother gets from an epidrual is very small. This dose of medication is slowly absorbed into the mother’s circulation over the next two hours and then broken down by the mother. The baby is not exposed to any significant amount of the drug. - “What should I do when in the middle of getting an epidural, a contraction comes?”
Most likely you have been cautioned not to move when an epidural is being administered. If you feel that a contraction is on its way, just let the doctor who is administering the epidural know and follow the instructions. You can be sure that you are not the first one who has a contraction during an attempt to insert an epidural. - “Someone told me that it took the doctor half an hour before the epidural was finally done. How could I cooperate so that the whole process is done as fast as possible?”
You can curl up and push your back out as much as possible. Some people curled up as instructed, but did not push the back out toward the doctor; the space between the spinal bones is still very narrow. You are asked to curl up for the epidural with the expectation that most people, when they curl up, push their back out.
Self-Help
Many methods of pain relief are simple, easy to do, costing very little, involving no needles or medicine, and because the participation of husband is needed, actually help to foster closer family bonds. How about:
- Listening to your favorite music, rocking yourself side to side with the rhythm of the music, humming the tune as you listen, adjusting your breathing patterns with the music… You can, of course, invite your husband to join you.
- Conscious relaxation during a contraction. You can tell yourself, or have your husband to remind you that you will cope with the pain. In between contractions, you will consciously check if your breathing pattern is back to a slower pace. Do a mental examination of your muscule groups, starting with your neck muscles. If you find tensed muscles, relax them. You can pull you body part in the opposite direction of the tensed muscle. For example, the muscles between the neck and shoulders are often tensed up under stress, you can flex your neck momentarily and then release the tension. It is very important to adopt a more tranquil pace between contractions because you have to recuperate and conserve energy for more contractions.
- Massage can help to lessen the pain during contractions and relax you between contractions. The usual massage techniques used to relief labor pain are rubbing and stroking. This is done by placing the hands flat on the area to be massaged and press lightly, rub and stroke the skin. The pressure used should be light as the purpose is not to move any internal structures, but rather to promote circulation. Massage in a circular motion can be done on the abdomen, the center of the back and the sacrum (an illustration will be inserted here) and on any tensed muscles. Massage in the low back and sacrum is particularly useful in the case of “back labor”, i.e. when the baby is facing toward your front, instead of your back. This positioning of the baby’s head often causes severe backache.
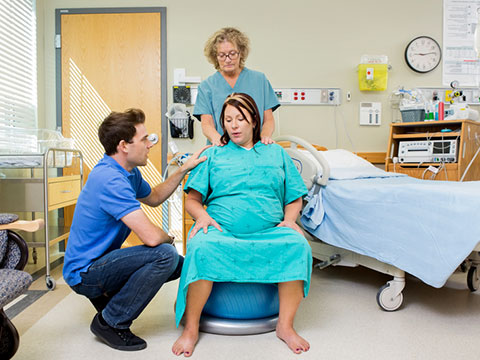
- Maintaining certain positions during a contraction helps many patients to cope with the pain. I have seen patients kneel while resting her head on a stool with her body upright, kneel forward on a pile of pillows, on all fours, sitting on a chair so that she can rest her head on a pillow over its back, standing and resting on her husband, lying on her side in bed, upright in a semi-squatting position while supported by her husband… You can essentially stay in any position as long as you remember 3 very important things:
- Never lie down flat on you back. The weight of the baby will compress blood supplies in your body and cause you dizziness and cause the baby to have less blood supply. If lying down flat is the only way that gives you relief, put a tilt on your body wit h a pillow underneath your right hip.
- The second point is that even if you are in a leaning forward position, try to stay as upright as possible as the purpose of the whole exercise is to have the baby moving down the birth canal.
- No matter what position you choose, even if you choose walking around in circles, do not arch your back.
Importance of the birth environment
It you are in a good mood, you can withstand pain better. As an expectant mother starts contractions, she is not only in pain, but also having the anxieties for the safe birth of her baby. At these crucial moments, sending her to a new environment where she will have to deal with a new group of strangers, as she experiences painful contractions every few minutes, does not seem to help her very much.
Recently, efforts were made to make the hospital environment as homely as possible. In advanced centers, the mother stays in the same room (the birthing room) for labor and delivery of the baby. (in contrast to the old way of moving the patient from the labor room to another room for the delivery). All of the medical equipment (suctioning, oxygen supplies, syringes, vials of medication) are stored inside cupboards fashions like kitchen cupboards. The bedding and the drapes, curtains, and furniture are chosen so that a homely atmosphere prevails. You may be encouraged to bring in your own linen, pillows, and clothing. Your family, including small children, are welcome to visit.
Some units have jacuzzi installed so that hydrotherapy (immersion in water) for pain relief is possible. It is felt by some that the buoyant sensation (literally so), and the fresh feeling of a tired body with perspiration being immersed in water promotes relaxation.